- Epilepsy is usually diagnosed by the careful description of recurrent events your child is having.
- Investigations may also assist in making a diagnosis.
Overview
- Epilepsy in children is usually diagnosed by a Doctor with training in epilepsy. In New South Wales, this would be through a Paediatrician.
- One of the most helpful tools for your Doctor is a detailed history of the seizure-like episodes.
- There will be very specific questions about the event.
- It may be helpful to complete the ‘Event Record’ and take it with you to your Doctor.
- If your child is having multiple events, you can record them on the ‘Event Diary’.
- Your Doctor will use this information along with any supporting evidence from investigations such as an electroencephalogram (EEG). An EEG is a non-painful test that records the electrical activity of the brain (see below).
- Sometimes your doctor will also perform blood investigations or imaging of the brain via an MRI (see below).
- If your child is given a diagnosis of epilepsy, your doctor will try and determine the cause.
- It is important to try and classify the type of epilepsy into a specific Epilepsy Syndrome. This helps with the understanding of treatment and prognosis.
EEG
- EEG stands for electroencephalogram
- (Electro = Electrical activity, Cephalo = Head, Gram = recording or picture).

About EEG
- Cells in the brain use very low levels of electricity to communicate with each other.
- In an EEG, a measurement of the electrical activity is shown on a monitor and appears as wavy lines.
- Small metal discs with wires attached are placed on your child’s scalp with some gel (this is painless). Some centres will use a cap rather than individual wires.
- The test will only pick up the electrical activity of the brain, it cannot read your child’s mind, nor does it give electric shocks.
- The wavy lines are read and interpreted by a specialist neurologist.
- The EEG findings are then considered along with the full medical history by the treating doctor who will decide a treatment plan for your child.
- An EEG takes approximately 30 mins.
EEG appointments
- You will be given instructions before your child attends their appointment as to whether they need to be kept awake for several hours prior to the test (sleep-deprived).
- Your child’s hair will need to be clean but no conditioner or oils should be used on the hair to enable the electrodes to stick to the scalp. Your child's hair also needs to be dry.
- To assist your child during the procedure, bring a toy or distraction that they can use while sitting in a chair. IPads, portable DVDs, books, colouring-in, or bubbles are often good choices.
- The EEG technician may ask your child to engage in some additional tasks during EEG monitoring, such as blowing a toy windmill (to bring on hyperventilation), asking them to look at flashing lights (photic stimulation), to open or close their eyes, or asking them to try to sleep.
- Once the recording has been finished you will be able to go straight home.
- The technician will give you information on how to best remove the gel from your child’s hair.
- Once the EEG has been reported, you will need to make an appointment to see your doctor for the results.
- A report of the results will be sent to your referring doctor, usually in about a week.
Video-EEG Telemetry:
- 'Telemetry' refers to two things being done at the same time.
- In Video-EEG Telemetry, both an EEG brainwave recording and a video recording of your child are made.

About Video EEG-Telemetry
- Video-EEG Telemetry involves the recording of a child’s physical activity with a video camera along with simultaneous brainwave (EEG) recording via a computer. It is used mainly in the diagnosis of events that are suggestive of seizures.
- Video–EEG telemetry is used to distinguish epileptic seizures from non-epileptic events.
- It is also used to help the doctor diagnose the type of epilepsy syndrome your child may have.
- If your child has an event while having telemetry, the doctors are able to review the video and corresponding brainwave recordings.
- If the recordings are indicating a seizure, characteristic patterns may appear in the brainwave recording.
Video EEG-Telemetry admissions
- During a Video-EEG telemetry admission, it is desirable for the patient to have their usual seizure events so these can be captured on the recordings.
- Staff will discuss options with the family to increase the likelihood of recording these events. This may include having your child engage in tasks likely to bring on their typical seizures, or having their medication doses temporarily altered. Your doctor will give you very specific instructions around this.
- If your child is booked in for a Telemetry study, it will most likely be done in a Children’s hospital.
- How long the study takes varies according to event frequency and other factors relating to the initial purpose of the study. The study may take several hours, overnight, or up to a week.
- Sydney Children’s Hospitals (Randwick and Westmead), only accept referrals from paediatric neurologists and paediatricians.
- One parent or guardian is required to stay with the child at all times.
- If staying overnight, the parent/guardian will have access to a bed in the room with the child.
- The Video EEG recording needs to be reviewed by a neurologist.
- The results will be discussed with you during the follow-up appointment.
MRI
- MRI stands for magnetic resonance imaging.
- It is a brain imaging device that uses a magnet and radio waves to take detailed pictures of the brain.
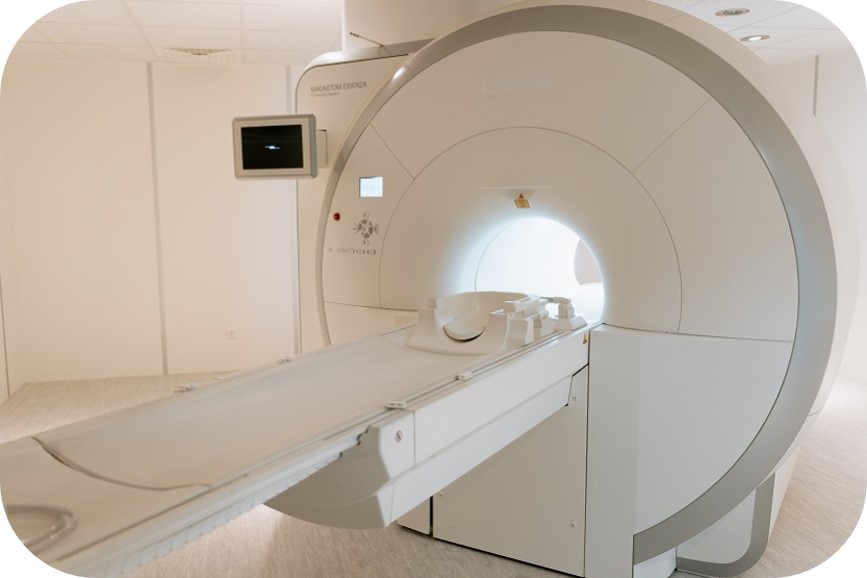
What does it involve?
- Your child will lie on a bed in a machine called an MRI scanner. It is a short tunnel, which is open at both ends (see image above). The bed is motorised and slides through the scanner.
- The MRI scanner is very noisy due to the magnet inside the machine being switched on and off. It is similar to a hammering sound. Your child will be given headphones to block out most of the noise, and they may be able to listen to music if available.
- Your child will usually be given a call button to use if they require any help while in the scanner.
- It typically takes approximately 45 minutes to have an MRI scan, but it can take up to an hour.
- Your child will have to lie completely still during this time. If your child is under the developmental age of around 8 years, or if you feel they are not able to lie still for this procedure or do not like confined spaces, your doctor may suggest a general anaesthetic.
- You will need to complete an MRI Safety Questionnaire to ensure there are no concerns with your child undergoing an MRI.
- The main areas of concern are if your child has any internal metal objects from previous surgery, such as a pacemaker. This is often not a problem for children.
- As the parent, you can be in the MRI room with your child, but also need to complete the Safety Questionnaire.
- If other children attend the appointment they will need to be supervised in the waiting area.
Risks
- If your child requires sedation or an anaesthetic, you may discuss the risks and benefits of this with your doctor.
How can you help your child?
- You can help your child prepare for an MRI by explaining the test in simple terms before the examination.
- Make sure to explain that pictures of their head will be taken.
- Let them know they will be in a small tunnel, and that the equipment will probably make knocking and buzzing noises.
- They will need to remain very still for the pictures. It may also help to remind your child that you'll be nearby during the entire test.
-------
Information last reviewed: 1/11/2022.